Inside UnitedHealth’s alleged scheme paying nursing homes to deny seniors hospital care

Could financial incentives be secretly influencing the care decisions for vulnerable seniors in nursing homes?
A recent investigation has shed light on claims involving the nation’s largest healthcare conglomerate.
An Investigation Uncovers Claims
According to reporting from The Guardian, UnitedHealth Group, a massive player in healthcare, allegedly used a controversial program within nearly 2,000 nursing homes nationwide.
The investigation, based on confidential records, interviews, and whistleblower declarations, details accusations of UnitedHealth inserting its own medical teams into these facilities.
The stated goal of this program, according to UnitedHealth, is to improve care and reduce unnecessary hospitalizations, which they argue can be costly and dangerous for elderly patients.
However, sources interviewed for the investigation tell a different story.
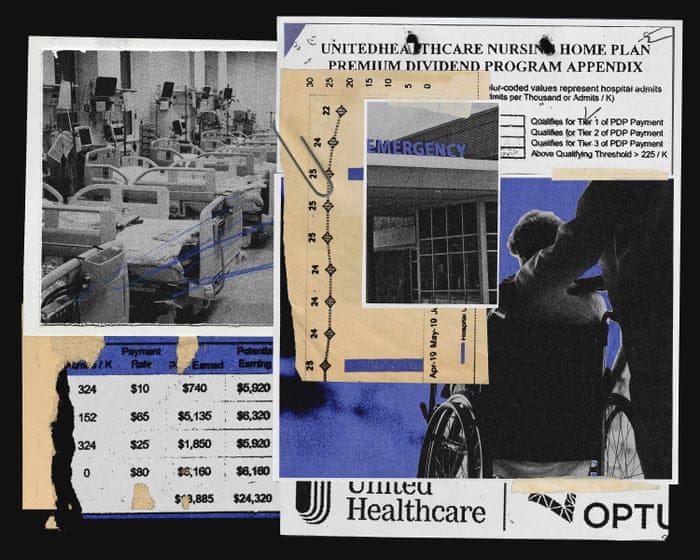
Allegations of Financial Pressure
The core allegation is that UnitedHealth secretly paid nursing homes thousands in bonuses.
These payments were reportedly tied to reducing hospital transfers for residents covered by the company’s Medicare Advantage plans.
Terms like “Premium Dividend,” “Shared Savings,” and “Quality and Shared Risk” were allegedly used to incentivize nursing homes based on keeping residents out of the hospital.

A key metric UnitedHealth executives reportedly focused on was “admits per thousand” (APK).
A low APK rate meant a nursing home was eligible for bonus payments. A high rate meant they received nothing.
“APK drove everything,” one former national UnitedHealth executive reportedly stated, speaking anonymously. “You gain profitability by denying care…”
UnitedHealth has strongly denied these specific allegations, stating that any suggestion its employees prevented hospital transfers “is verifiably false.”
They maintain that their bonus payments and partnerships help prevent unnecessary hospitalizations and ultimately improve health outcomes for residents.
Cost-Cutting Tactics Explored
Beyond direct bonuses, the investigation touches on other alleged cost-cutting tactics within the program.
This included supervisors allegedly giving teams “budgets” for hospital admissions.
There are also claims that the company monitored facilities based on the number of residents with “do not resuscitate” (DNR) orders.

Several current and former UnitedHealth nurse practitioners reportedly alleged managers pressured them to persuade patients or their families to change their code status to DNR, even if it wasn’t the patient’s expressed wish.
UnitedHealth denies inappropriately pushing patients to change their code status.
They reiterate that their program provides valuable resources like on-site practitioners and tailored care plans.

Additionally, the investigation claims the program offered larger payments for enrolling seniors into specific long-term nursing home Medicare Advantage plans.
This allegedly led to some nursing homes sharing confidential resident information with UnitedHealth sales teams.
One whistleblower lawsuit reportedly details how nursing home staff were incentivized to leak records for sales pitches, sometimes resulting in seniors being enrolled without full cognitive capacity to consent.
UnitedHealth declined to answer specific questions on the total amount of payments made but stated they incentivize high-quality outcomes and improved care.

Specific Cases Raise Concerns
The investigation highlights several specific instances where UnitedHealth’s intervention in nursing home protocols allegedly led to delayed hospital care.
In one reported incident from 2019, a resident in Renton, Washington, showed possible stroke symptoms.
Despite the nursing home nurse recognizing potential stroke signs, a remote UnitedHealth provider allegedly suggested a less serious condition and advised waiting for blood test results and a follow-up in four hours, instead of immediate transfer.
The patient’s independent doctor was reportedly not informed of this delay.

Another case from Puyallup, Washington, reportedly involved a nursing home nurse delaying a resident’s transfer due to UnitedHealth protocols requiring guidance from the company.
The delay, estimated at about an hour before the resident was eventually transferred by their independent doctor, allegedly resulted in the patient suffering permanent verbal slurring and facial droop.
UnitedHealth declined to comment on specific patient cases, citing confidentiality. However, they noted that transfer decisions involve many factors, including patient goals and input from the care team, and the company does not prevent facilities from contacting independent doctors.
Former UnitedHealth nurse practitioner Maxwell Ollivant, who filed a congressional declaration and previously a lawsuit (which the DOJ declined to intervene in), has become a whistleblower.
Ollivant has urged lawmakers to ensure that UnitedHealth is not “skimping out on care” and that patients receive the services they need when the time comes.
UnitedHealth contends that Ollivant lacks the necessary data and expertise to assess the program and points to the DOJ declining his prior suit after a multi-year investigation.
Continued Scrutiny
The claims raise questions about the influence of financial incentives in healthcare decisions, particularly for vulnerable populations in long-term care settings.
While UnitedHealth maintains its program improves care and prevents unnecessary hospitalizations, the investigation’s findings suggest a need for continued examination of such practices.